
Hundreds of thousands of dementia sufferers risk missing out on “life-changing” treatment after diagnosis rates plunged during the Covid pandemic, campaigners have warned.
Every region of England has missed the national diagnosis rate target of 66.7 per cent for the past two years, analysis by The Independent shows.
Rates are calculated by comparing recorded diagnoses with the estimated prevalence of the disease. As of September this year, there were 437,236 people aged 65 or above diagnosed with dementia in England. The NHS estimates that there are around 703,000 people in England living with the illness, meaning that approximately 266,000 are believed to be undiagnosed.
Diagnosis rates reveal a postcode lottery for patients, with performance declining across the country since 2019-20, and South West England faring most poorly. Scotland, Wales and Northern Ireland do not routinely publish the equivalent data.
Have you been affected by this story? If so, email matt.mathers@independent.co.uk
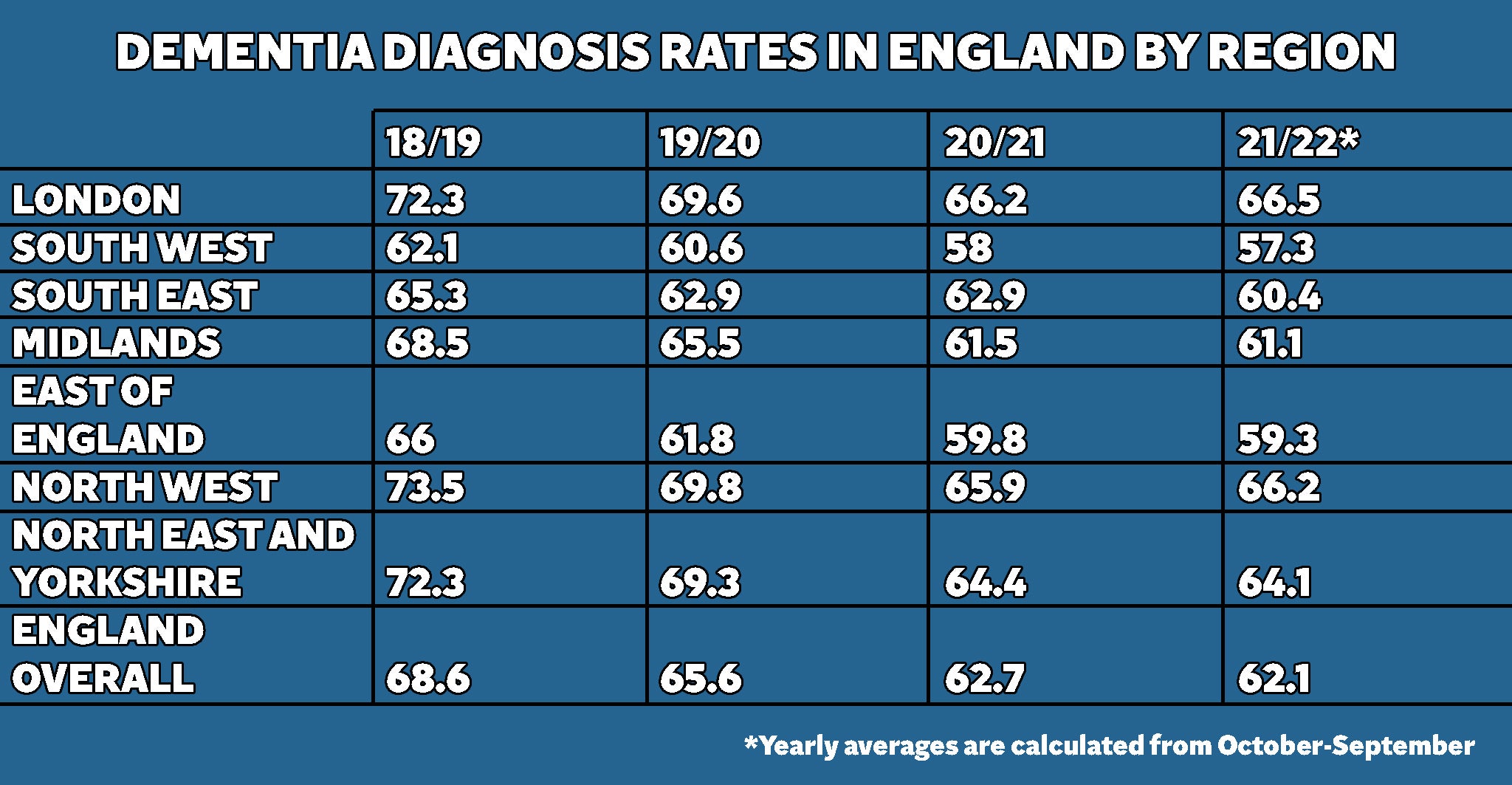
South West England had an average diagnosis rate of 57.3 per cent in the 12 months from October 2021 to September 2022 – the last month for which NHS figures are available.
NHS England has paused publishing the monthly data until January 2023. Officials said this was because of changes in the way the data was being collected.
The two best-performing regions – North West England and London – recorded averages of 66.2 and 66.5 per cent respectively in 2021-22, but still missed the target introduced by David Cameron 10 years ago.
Diagnosis rates were already declining across England in the year before the pandemic, and have continued to do so in every year since. The last time any region hit the national target was in 2019-20, with only London, the North West and the North East attaining a level above 66.7 per cent.
The reason for the disparity between regions is unclear. Officials at South West England NHS were unable to explain why diagnosis rates were particularly low there.
Nationwide, the Covid pandemic has severely affected diagnosis rates, campaigners and the NHS say.
People with suspected dementia are given cognitive tests, usually by a GP, to check their mental capacity. Often the final step in the diagnostic process is a brain scan, once simpler assessments – such as blood tests – have ruled out other problems.
But many people stayed away from GP surgeries at the height of the pandemic for fear of catching the coronavirus, and rates have yet to improve despite restrictions having ended early in 2022.
Lockdowns have contributed to huge backlogs in GP appointments and referrals to diagnostic services. NHS figures published in October show there were 184,000 patients in England waiting three months or longer for tests.
Despite an additional £17m being released to clinical commissioning groups in June 2021 to improve the process of diagnosing dementia, the average rate for England in September 2022 was still below target, at 62.2 per cent. This was up only slightly from 62 per cent in the previous September, and still well below the 68.8 per cent recorded in September 2019, prior to the pandemic.
Susan Mitchell, head of policy at Alzheimer’s Research UK, said the situation has “clearly not improved” in recent months despite the cash injection given to frontline diagnostic services.

She said that while it was “much harder” to get a dementia diagnosis during the pandemic, there was already a “lack of capacity” in the system before the virus struck.
“The government must renew its focus on improving how people with symptoms of dementia are diagnosed as a matter of urgency,” Ms Mitchell said. “The time between referral and diagnosis can be as much as two years. During this time, the underlying diseases which cause dementia can worsen significantly. This is unacceptable.
“At a time when new treatments for dementia are on the horizon, it has never been more important for people to be diagnosed quickly and accurately. Failure to improve diagnosis rates could result in many people missing out on potentially life-changing medicines when they are available.”
Trina Armstrong, 76, from north London, waited four years for an accurate diagnosis of a rare form of Alzheimer’s disease. She first noticed that something was wrong in 2006 when she began having trouble recognising faces and reading telephone numbers.

Following a CT scan in 2009 she was told she’d probably had a stroke, which surprised her and her husband Graeme. The couple said they hadn’t recognised any symptoms of a stroke.
In September 2012, Ms Armstrong was referred to a specialist clinic for visual loss after a stroke or brain injury, where a doctor suggested she might have a degenerative disease.
She was finally diagnosed with posterior cortical atrophy, a rare form of Alzheimer’s disease that affects the back of the brain.
Mr Armstrong said it is vital that more money and research is invested in diagnostic services. “Had we had an accurate diagnosis four years earlier, Trina could’ve been placed on the correct medication, which may have been more effective and helped her day to day,” he said. “We would also have been able to access support sooner.”
He added: “Compare this to my diagnosis of early-stage prostate cancer, which was diagnosed, treated and effectively cured in four months. This is why we need more research into diagnosis. If we can do this for cancer, we can do this for the brain diseases that cause dementia.”
Dementia, which affects around 850,000 people in the UK, is a syndrome associated with an ongoing decline of brain function. There are many different causes of dementia, and many different types, including Alzheimer’s.
A study published in September found that a drug slows cognitive decline in patients with early stages of Alzheimer’s, in what was hailed as a major breakthrough for the treatment of the disease.

Mr Cameron launched the dementia challenge in 2012 when he was prime minister, setting a target to achieve an average diagnosis rate of 66.7 per cent by 2020. Successive governments have committed to trying to reach the target, which has been described by Alzheimer’s Research UK as “modest”.
In August, Boris Johnson launched a new “national mission” to tackle dementia, in memory of the late Carry On and EastEnders star Dame Barbara Windsor. Mr Johnson said the government would commit an additional £95m in research funding, meeting a manifesto commitment to double the funding of Alzheimer’s research to £160m by 2024.
James White, head of public affairs and campaigns at Alzheimer’s Society, said it was “concerning” to see that there is still “drastic variation” in diagnosis rates across England. “While the Covid-19 pandemic had an impact on reducing diagnosis rates, they must return to pre-pandemic levels as a minimum,” he said.
Mr White added that ministers must do more to remove the “current postcode lottery experienced by many when seeking a dementia diagnosis, ensuring equitable access for all, regardless of locality”.
“The sooner people with dementia get an accurate diagnosis, the sooner they can access the support they need,” he said. “The government promised a 10-year plan for dementia in May, but we’ve since received 22 responses from them stating the plan will be delivered ‘in due course’.”
He added: “The government should seize the hope and opportunity that research advancements have presented, by urgently delivering the plan and developing tangible solutions to the problems with our diagnosis processes.”
An NHS England spokesperson said the pandemic had had an impact on people’s mental health, and that some older people may not have sought help for symptoms of dementia, although referrals to memory clinics had increased.
“The NHS is improving support for people affected by dementia, their families and carers, by providing more personalised care packages. With early diagnosis so important, if you or a family member think something is not quite right, please come forward as soon as possible,” the spokesperson added.
NHS England has commissioned the Dementia Intelligence Network, part of the Office for Health Improvement and Disparities, to investigate the underlying variation in dementia diagnosis rates in targeted areas across England.
A Department of Health and Social Care spokesperson said: “During the pandemic, memory assessment services were temporarily suspended, which contributed to a fall in diagnosis rates. These services have resumed and are offering a more personalised approach for patients – with telephone, video conference and face-to-face appointments being provided.
“We made £17m available to clinical commissioning groups last year, to tackle waiting lists and increase the number of dementia diagnoses as well as providing support to patients both before and after diagnosis. We are reviewing plans for dementia in England, and further information will be available in due course.”








