Lianne was just 13 when she lost her parents to Aids. Newly orphaned, she had to find a way to keep herself and her younger sister alive. With no money to finish school, unable to find a job and struggling to put food on the table, there was only one option – sex work.
Now 24, she knows the dangers in Eswatini, a kingdom in southern Africa once described as the epicentre of the HIV epidemic and a country still struggling with some of the highest infection rates in the world.
“Both my parents passed away. Hunger led me to join this work although I know it’s risky,” Lianne says, explaining that she earns under £25 a week. She is unable to acquire HIV preventative medication – known as PrEP – on her own.
But there is now hope in the form of lenacapavir – dubbed the “miracle” drug – which the United Nations hopes can protect millions of people like Lianne and even end the Aids epidemic altogether.
The twice-yearly injection – described by the head of the UN Aids agency as “the closest thing we have to a vaccine” – provides near complete protection against infection.
Lenacapavir is being introduced for the first time in nine of the most at-risk countries, including Eswatini, meaning Lianne was among the first people in the world to get the injection.
While it is a big step forward in HIV care, concerns have been raised about the extent of the rollout and fears it will be ineffective if it is not introduced on a global scale.
The positive news about lenacapavir comes after last year’s devastating cuts to foreign aid spending by US president Donald Trump, which had previously funded around half of Eswatini’s HIV response.
For Lianne, it meant the abrupt closure of the mobile clinics that gave her access to potentially life-saving HIV prevention therapy for free.
The closures have had a deadly effect: a friend and fellow sex worker recently died after contracting HIV and losing access to life-sustaining medication.
“That is why I am so happy today, it’s protection,” she continues with relief, as she receives the brightly coloured yellow injection.
At the beginning of 2025, the world was on track to end the Aids pandemic by 2030.
But that was upended by unprecedented foreign aid cuts from the US, the UK and other European countries, which have created the biggest ever disruptions to HIV response, from testing to treatment and prevention.
If these aid cuts continue, there could be millions more deaths and infections, as well as double the number of medication-resistant strains, according to The Independent’s own modelling of data.
This makes the timing for the lenacapavir rollout critical. Developed by California-based biopharmaceutical company Gilead Sciences, the UN believes the treatment, if properly deployed, could help bring about the end of the epidemic by reducing new infections to zero.
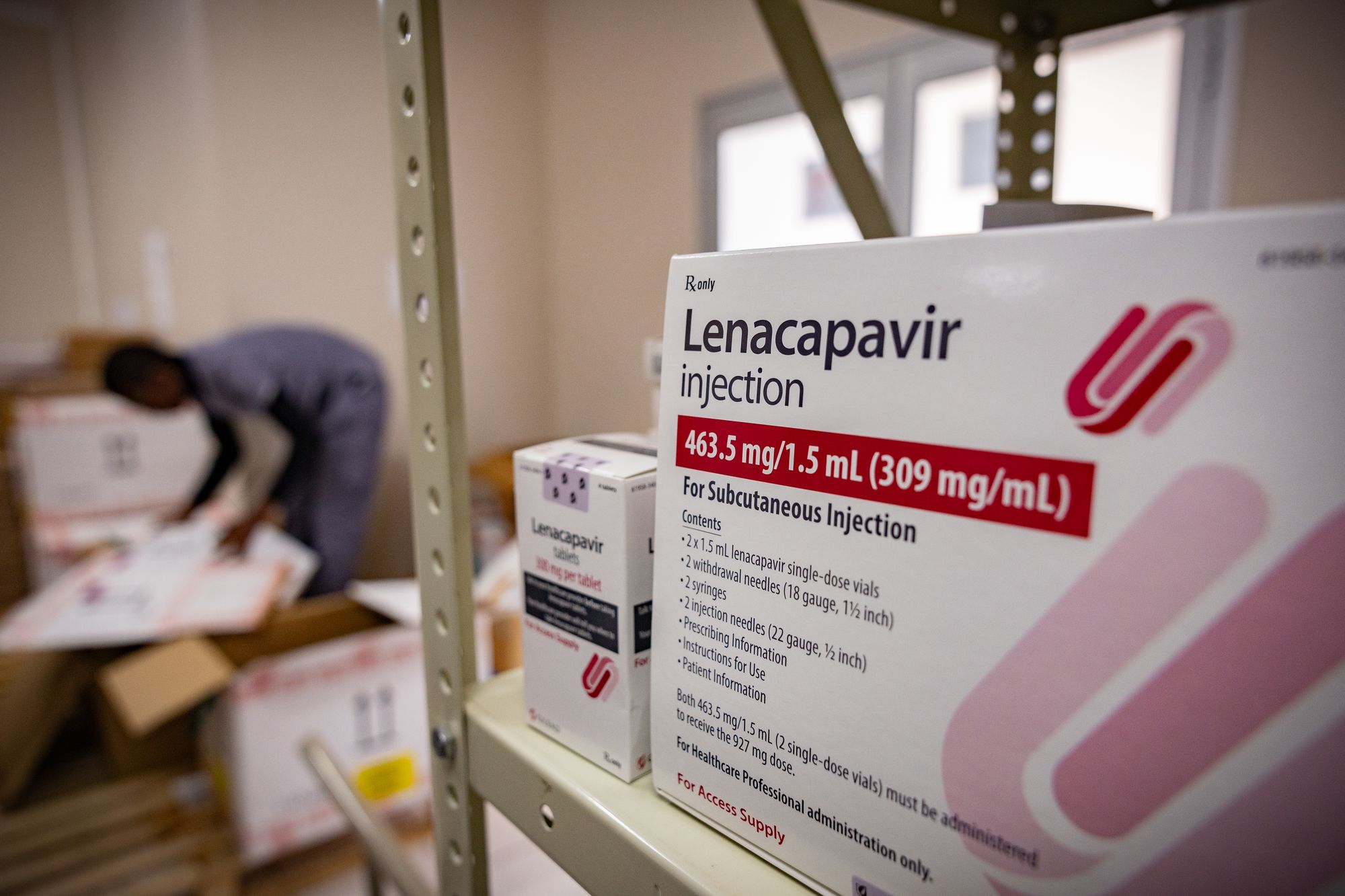
The current plan, funded by the Global Fund to Fight Aids, TB and Malaria, together with the US government and others, is to deliver lenacapavir to three million people by 2028.
Lenacapavir, which in wealthy countries can cost up to $24,000 (£18,000) a year, is being simultaneously delivered to some of the poorest countries most at risk at a significantly reduced cost.
Life-sustaining antiretroviral therapy was infamously accessible in the West for a full decade before being rolled out in sub-Saharan Africa, costing countless lives and paving a way for the crisis today.
“This has been a defining moment for the Aids epidemic,” says Dianne Stewart from the Global Fund. “We have been fighting for equitable access to new tools since the beginning, and this is the first time in history that we have got it right.”
The first country to receive these jabs is Eswatini. Formerly known as Swaziland, it has worked hard to reduce new HIV infections from a peak of 21,000 per year 20 years ago to 4,000 in 2023, according to the UN.
But still around a quarter of Swazis aged between 15 and 49 are living with HIV, according to the latest data from the US Center for Disease Control.

David Maseko of HealthPlus for men, a charity working with key populations including LGBT+ communities, explains that the aid cuts shut all 15 mobile charity clinics that Lianne and others used.
That has meant there has been a soaring number of people – including some of the most at-risk communities – off their HIV medication and off PrEP – a problem unfolding across Sub-Saharan Africa.
“There are a lot of gaps now. We are even struggling to do community testing.”
For him, a twice-yearly injection that could help curb the recent surge in infections is “simply a game-changer”.
Arianna, 17, who was also forced into sex work after her mother died and she left an abusive home, agrees. “This is lifesaving for us,” she says as she gets the injection.
She explains that trying to get daily prevention PrEP pills from a public facility, where she could face prejudice as a sex worker, makes it near impossible, especially when they earn so little a week to cover transport.
“That is why today I decided to come here. To me, this is the best way to help myself, to survive.”
But there are concerns that without proper investment around the world to reach a critical mass of people protected globally, the impact will be limited.
For now, delivery is targeted at just nine countries, although there are plans to expand that. Lenacapavir has not yet been licensed or procured for delivery in large parts of Latin America, where infection rates are rising.
“We have seen in the past that piecemeal solutions, especially for infectious diseases, do not work,” adds Stewart from the Global Fund.
“As we saw during Covid, you cannot solve it in one country and think it is done while others do not have access.”
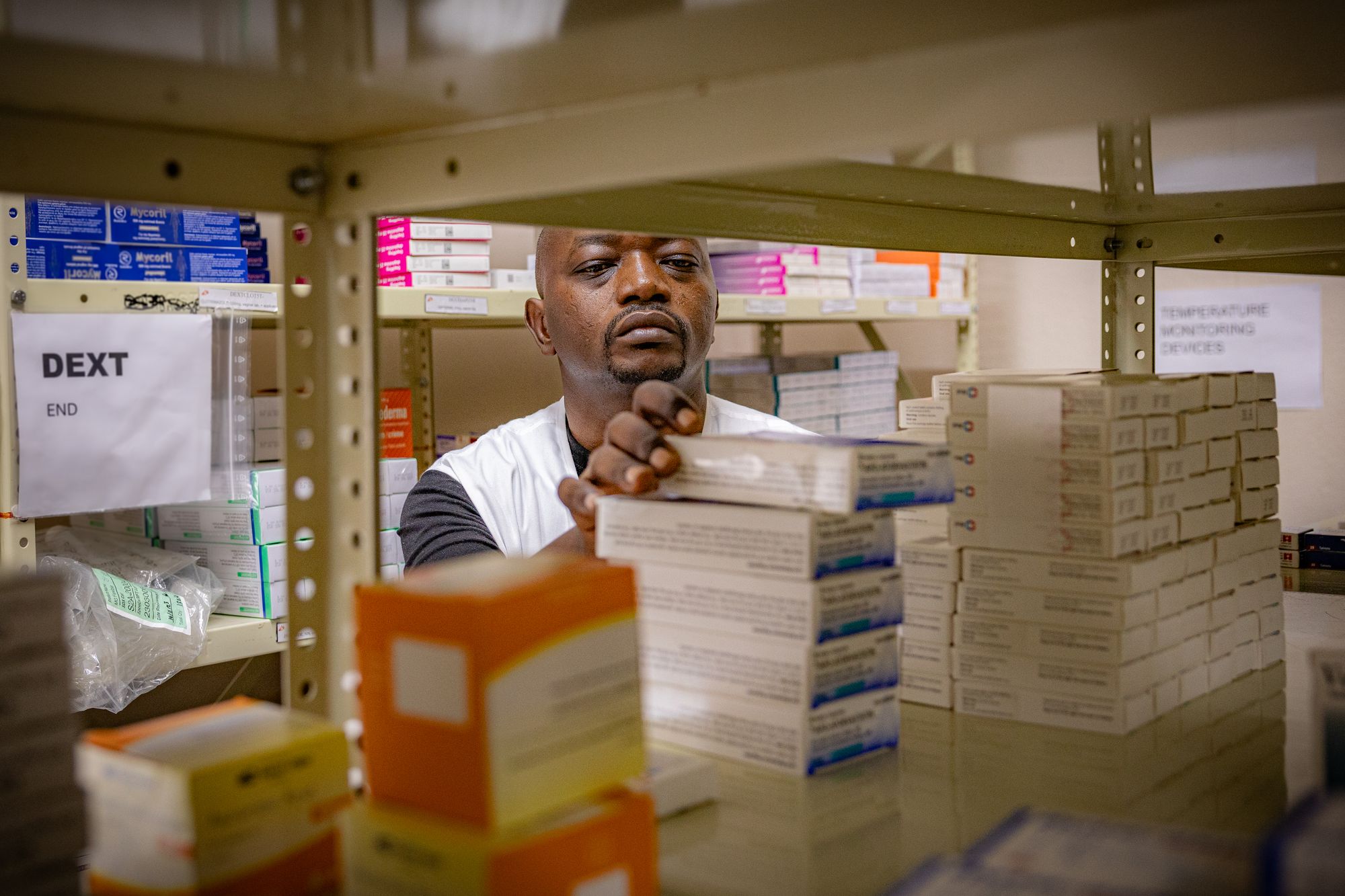
At a Medecins Sans Frontieres (MSF) clinic in a town outside the capital, country lead Dr Diojki Bahati says they were given only 50 doses to distribute and have had to turn patients away.
Even reaching two million people with lenacapavir over the next three years is “far below the global need”, he continues.
UNAIDS has said that to tackle the pandemic, the world needs to get 20 million people on PrEP in the next few years.
“Two million people over three years is less than 10 per cent of that target.”
He adds that there are no alternative procurement systems, especially for organisations like MSF, that he says have been denied the right to purchase directly.
In parallel, generic manufacturing licences have been granted to around six manufacturers in the coming year to supply 120 countries and territories.
“But that leaves quite a number of low- and middle-income countries where up to 20 per cent of new infections are happening,” he continues, such as Brazil, Peru and Mexico that participated in lenacapavir drug trial.
He says it is essential that the rollout is properly funded and supported by governments, even as they cut aid. It will ultimately be considerably cheaper in the long term.
In 2024, there were at least 1.3 million new HIV infections. Carmen Pérez Casas, from health initiative Unitaid, explains that these additional infections will cost an extra $52m (£38.8m) per year if everyone is put on antiretroviral treatment, leading to a lifetime treatment cost of approximately $2bn.
As transmission increases, this cost will accumulate exponentially over time.
“Delivering Lenacapavir to prevent infections would be a fraction of this cost,” she adds.
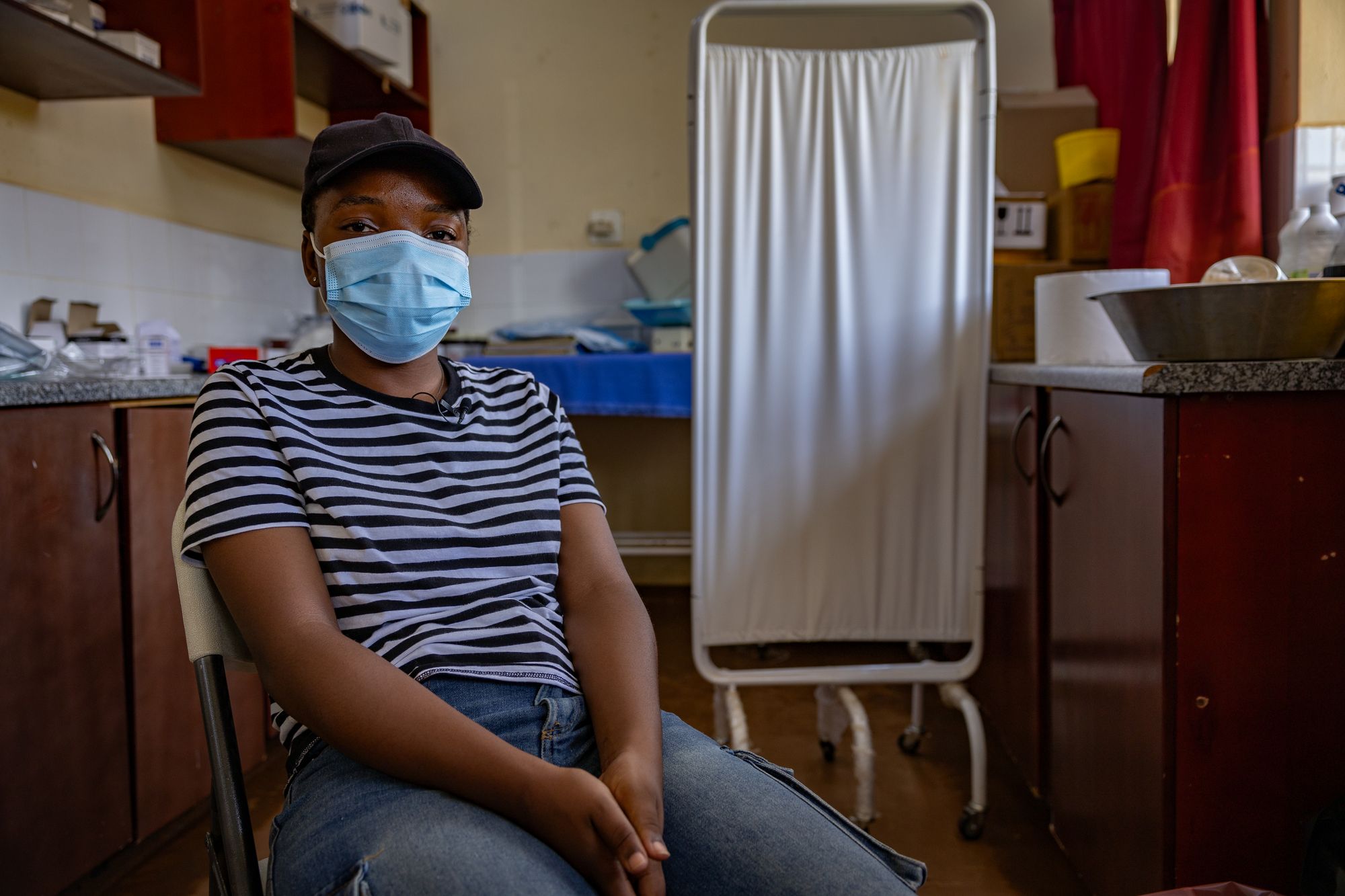
Back in the Eswatini clinic, the demand is clearly there. Lianne and Arianna breathe a sigh of relief after getting their jabs, knowing for now they are protected.
“We beg that they do not get tired of helping us,” says Lianne as she finishes her appointment. “If they are cutting the funding, it means we will be exposed and die of HIV. Please help.”
This article has been produced as part of The Independent’s Rethinking Global Aid project
‘We’re going to lose so many girls’: The deadly impact of Trump slashing aid for contraception
The Aids crisis was set to end by 2030 – now Trump’s cuts will mean 4 million more deaths
Death Sentence: The real cost of Trump’s aid cuts on HIV
Inside the battle to end the Aids pandemic in the face of Trump’s cuts
Project Freedom pulled and Operation Epic Fury over: Inside Trump’s 48 hours of chaos
Pope Leo hits back at Trump over claim he is ‘endangering Catholics’
Iran-US war live: Tehran and US ‘closer than ever to agreeing memo to end war’






