MUMBAI: The insurance ombudsman on Wednesday directed National Insurance Company to pay Rs 82,785 to a claimant who had undergone a cataract operation and whose claim had been partly paid.
The ombudsman said the insurer’s reasons that the expenses related to the treatment for correction of eyesight due to refractive error less than 7.5 diopters (measure of lenses’ power) and the amount was not reasonable, was unjustified.
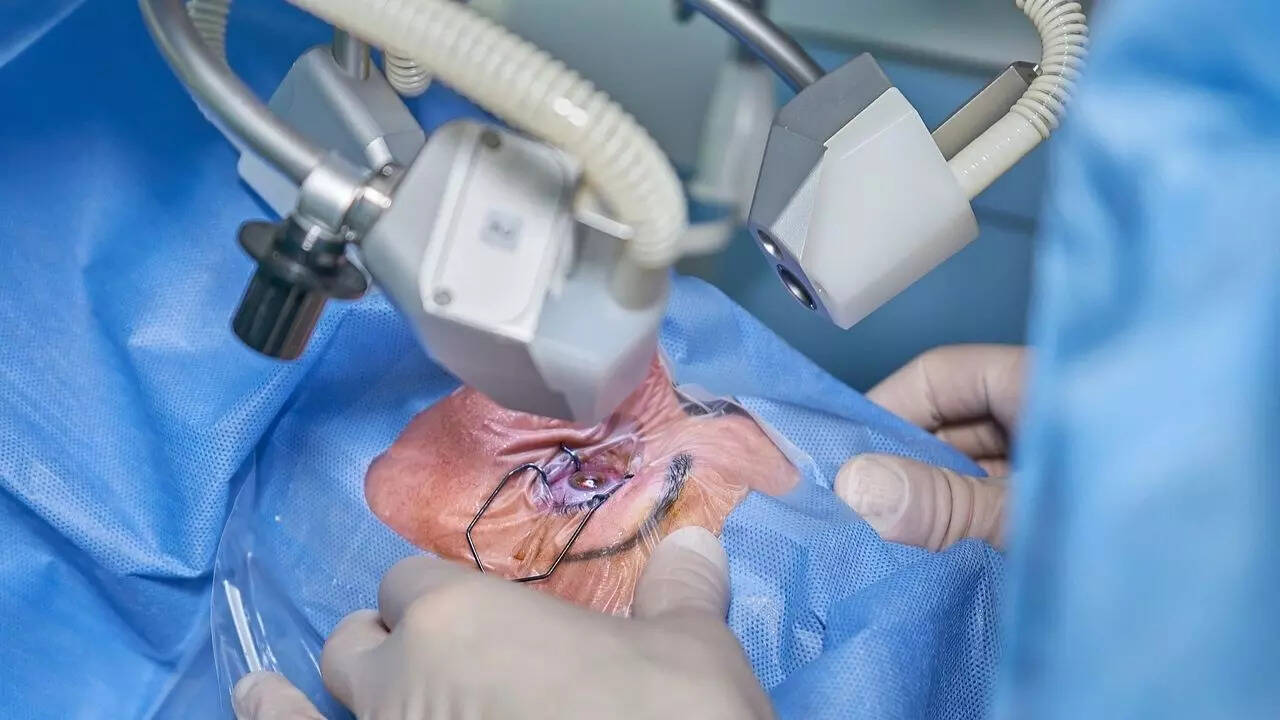
Sridhar Ramamurthy had undergone cataract surgery (phacoemulsification) with intraocular lens implant for both the eyes in May this year at Shanmukhananda Eye Care Dept and lodged claims for an amount of Rs 1,44,060 with National Insurance Company.
The claims for both the eyes were partially settled for Rs 61,275 and Rs 82,785 was rejected citing various reasons, including the reasonable and customary expenses clause.
Responding to a query filed under the Right to Informaton Act (RTI) by Ramamurthy, NIC said the claim was rejected because a bifocal lens was used for correction of refractive error.
“Cataract surgery is aimed at removing the cloudy lens from the eye and replacing the same with Intra Ocular Lens (IOL) and restoring clear vision. The monofocal lens is adequate to treat this condition; multifocal lenses correct the refractive error along with treating the cataract condition. Correction of refractive error less than 7.5 diopters is excluded from the scope of the policy,” the company said in its response.
The treating doctor had said that the refraction in the patient's right eye was -7.5/+0.25x90 and the left eye -6.5/+0.25x40.
“Being an employee of the Bank of India he has to work continuously on the computers and handle figures for which a fine vision is necessary. He was suggested different types of lenses along with the cataract surgery and the option of the multifocal lens was given to him which would help him professionally”.
The policy was a group health cover for Bank of India which was by National Insurance. The insurer’s representatives were absent for the hearing.
Citing the insurer’s reasons as unjustified, the ombudsman said, “Under the facts and circumstances of the case, National Insurance Co Ltd is directed to settle the above claim for the balance amount of Rs 82,785/- barring non-medicals, if any, in favour of the Complainant within 30 days from the issuance of this order.”