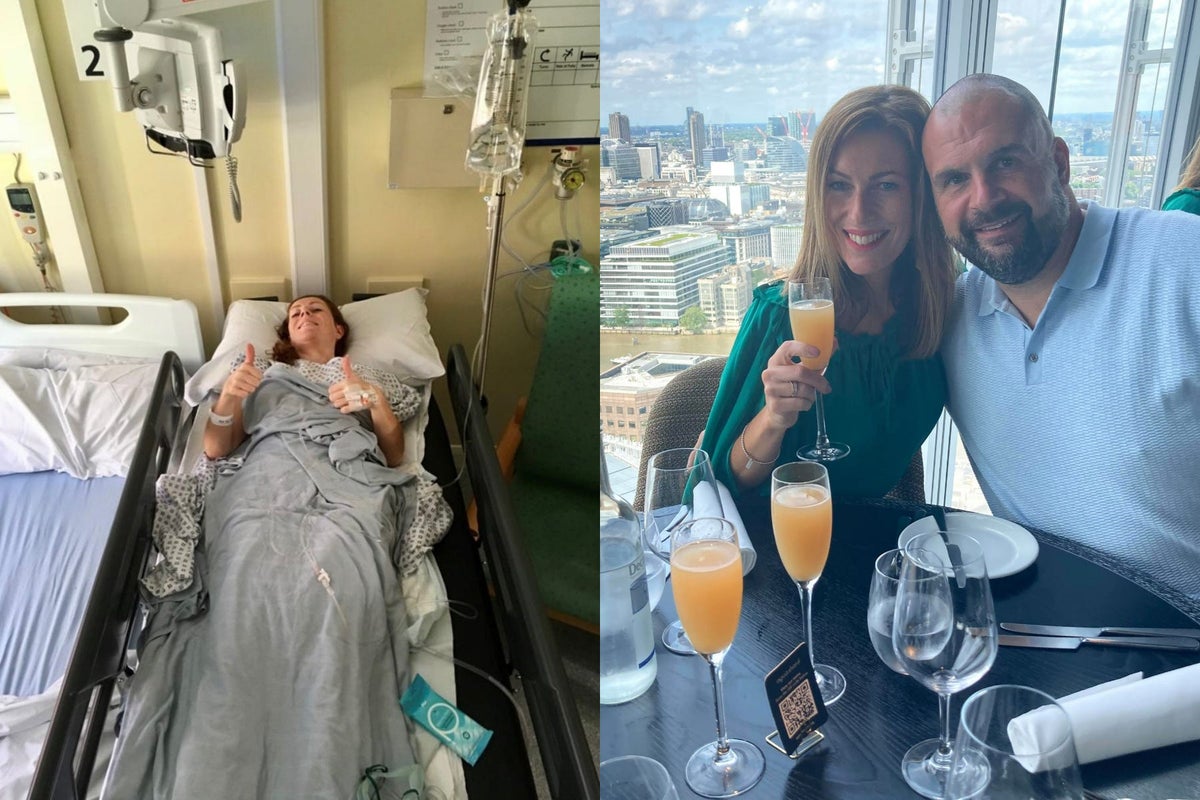
A cancer survivor who experienced severe vaginal bleeding which felt like “somebody had just popped a balloon”, before she underwent gruelling treatment to remove a large vascular tumour in her cervix, wishes to give the positive message to other women that a cervical cancer diagnosis is “not a death sentence”.
Joanne Painter, who lives in Northampton, was diagnosed with stage 2 cervical cancer when she was 38 years old after noticing unusual vaginal discharge and then experiencing abnormal, heavy bleeding for several months.
The mother-of-two, who is the founder and managing director of a natural green burial ground and a humanist funeral celebrant, said the bleeding was so severe that, on occasions, it felt like “somebody had just popped a balloon or turned the tap on”.
The now 43-year-old said she was repeatedly told by doctors that they were not concerned and was initially misdiagnosed as having a cervical ectropion – when cells from inside the cervical canal grow onto the outside of the cervix – but Joanne knew her symptoms should not be ignored.
After pushing for a diagnosis, in February 2018, Joanne received the news she had cervical cancer and said she was “dumbfounded” – but now, as a survivor looking back on the last five years, Joanne wants to raise awareness of the importance of early detection and “remaining positive”.
“You know your body better than anyone and, if something’s not right, then don’t be fobbed off by a practitioner or a doctor, or whoever is saying ‘oh, it’s fine’… keep going and get screened and get vaccinated, if you can, and don’t take no for an answer,” Joanne said.
“Obviously, the sooner you can get a diagnosis, the better chances you are going to have.”
Cervical cancer is a cancer that is found anywhere in the cervix – the opening between the vagina and the womb – and, according to the charity Jo’s Cervical Cancer Trust, it currently kills two women in the UK every day.
A cervical screening, known as a smear test, checks the health of the cervix and is a test to help prevent cancer, but in Joanne’s case, the results from her previous smear tests were negative prior to her diagnosis.
After noticing unusual discharge at the age of 38, which she described as “very watery”, Joanne contacted her GP to arrange an appointment.
She said the doctor “wasn’t very concerned at all”, but just days later, she started to experience vaginal bleeding, which progressively worsened.
Joanne likened the bleeding to a “light period” at first and was initially diagnosed as having a cervical ectropion, but when she started to bleed through her sanitary pads to her clothing and was spending up to an hour on the toilet at times, she knew “this isn’t right”.


It became so severe that, during a trip to the theatre with friends, she said she “felt this ‘pop’ and there was blood gushing down (her) legs”.
On another occasion, during a trip to Australia, she bled “for nearly the whole 24-hour flight” and it “came through to the airplane seat”.
Joanne said: “The spotting became really heavy bleeding; I could sit on the toilet for 20 minutes at a time and it was like somebody had just popped a balloon or turned the tap on, and it was just, drip, drip, drip.
“That was when I started to think, ‘oh, this doesn’t seem right’, and at that time, I was feeling really, really tired.
“I had a four-year-old and a seven-year-old, I was working full time, so I just put the tiredness down to that…(but) obviously, I was losing quite a lot of blood, so that led me to go back to my doctor again.”
Joanne was referred to a genealogist at Northampton General Hospital, but her husband Neil, 48, a builder, took her to the hospital earlier, as she ended up bleeding through her clothing again while out for dinner.
She said doctors were initially dismissive of her symptoms once again, but after staying overnight to try to stop the bleeding, Joanne was told by a gynaecologist consultant the following morning: “I’m really sorry, this doesn’t look good.”

She was informed she had cervical cancer and, after a biopsy had been taken and she underwent various scans and an MRI, it was revealed she had a 6cm vascular tumour in her cervix, which would require treatment rather than surgery to remove.
“I was totally and utterly in disbelief, to be honest… I remember just sitting there, just completely speechless,” Joanne said.
“I wasn’t upset particularly, I think it was just like, is this actually happening?
“Then, within about half an hour, a Macmillan nurse just appeared at the bottom of my bed and introduced herself, and I think that was the moment that it sunk in – the reality of, oh my God, I actually have a Macmillan nurse sitting at the end of my bed, that is not good news.”
Joanne explained that the news was even harder to hear as she had lost her dad to cancer nine years earlier, but despite her fears, she knew she had to stay positive.
“I was sitting there, thinking, my dad died of cancer, now they’re telling me I’ve potentially got cancer, and I’ve got a four-year-old and a seven-year-old, and I’ve got to get through this because I can’t not be there for my children,” Joanne explained.
“So very quickly, this overwhelming need to survive just came over me.”
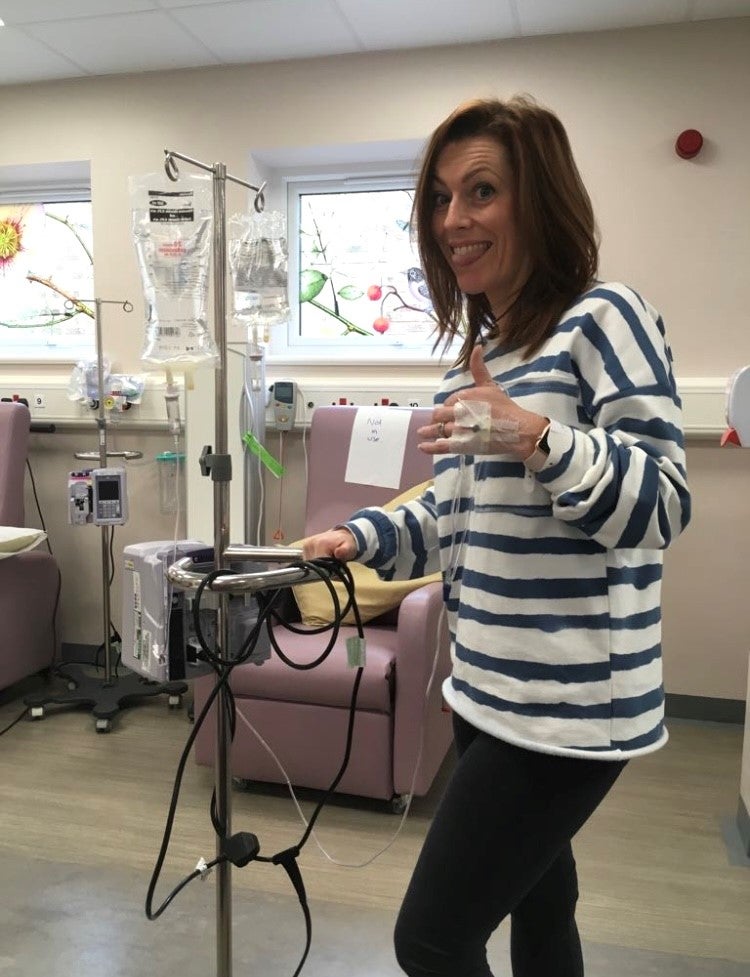
Joanne believes that her positive mindset was fundamental in helping her get through her treatment, which involved six weeks of chemoradiation followed by three weeks of brachytherapy – a type of internal radiation therapy, which Joanne said left her insides “black and chargrilled”.
The mum-of-two explained that she did not lose her hair, due to the type of chemotherapy she underwent, but she felt “dreadful” at times.
She said she experienced severe exhaustion, chronic diarrhoea, and felt “a bit hungover, like (she had) done 20 shots of tequila”, and even though she was “terrified” at times, she knew she had to push through the challenges she faced, especially for her children.
“You can’t dwell on it, you’ve just got to get on with it,” Joanne said.
“You never want (your children) to see you upset and you never want them thinking you’re that poorly, so you just crack on…
“I never felt like I needed any counselling, I didn’t want anybody to feel sorry for me; I didn’t want to ever be defined as ‘Jo who had cancer’, so I was very much like, just get on with this, get through it, it’s not that bad.”
Three months after her treatment had ended, Joanne went back to the hospital for a check-up and was given the “wonderful” news that the tumour had gone.

Although Joanne said it took “a long time to recover” and described the after-effects of her treatments, such as going into menopause, as a “train crash”, she stressed the importance of having a good support network, exercising, and “being kind to yourself” during rehabilitation.
Joanne is also a “real believer in the law of attraction and putting it out to the universe”, and she said writing affirmations helped enormously.
“These things do take time, so people need to probably just know that (they’re) not going to bounce back and feel absolutely 100% afterwards and life go back to normal,” she said.
“I think there is a bit of a life adjustment and just accepting the new you; this is ‘the new me’ now, and I am different to what I was beforehand, but it’s not a bad thing, it’s just slightly different.”
Joanne has regular check-ups every few months and although she has had a “few wobbles over the years”, she wants to encourage other women who may have had a cervical cancer diagnosis to “try not to go down that fear tunnel of ‘this is a death sentence’,” adding: “You’ve got everything to live for.”
Cervical Cancer Prevention Week runs from January 23-29 and Jo’s Cervical Cancer Trust is launching its biggest ever campaign: #WeCan End Cervical Cancer, to work towards a day where cervical cancer is a thing of the past.
You can find out more by visiting the website here.








