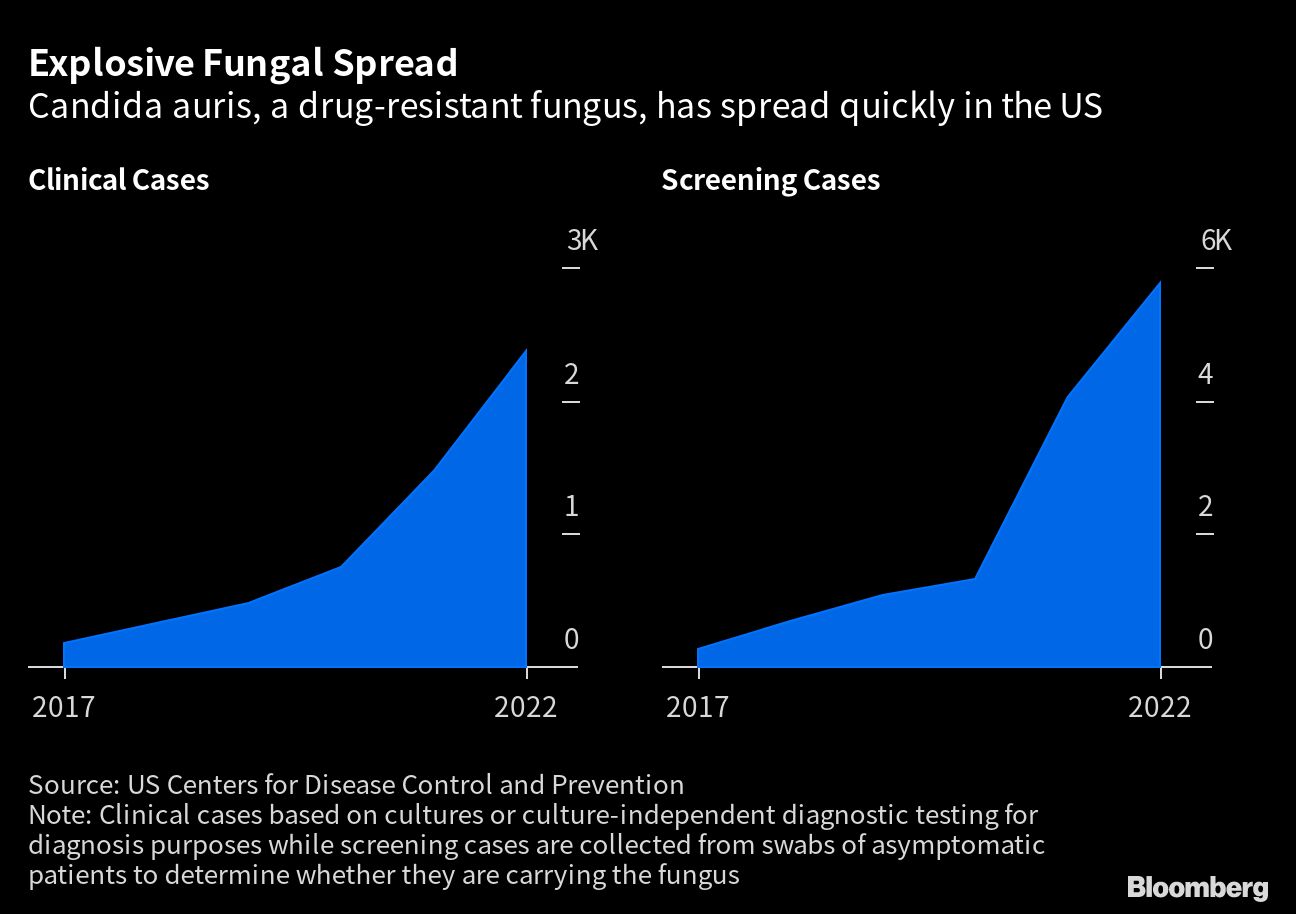
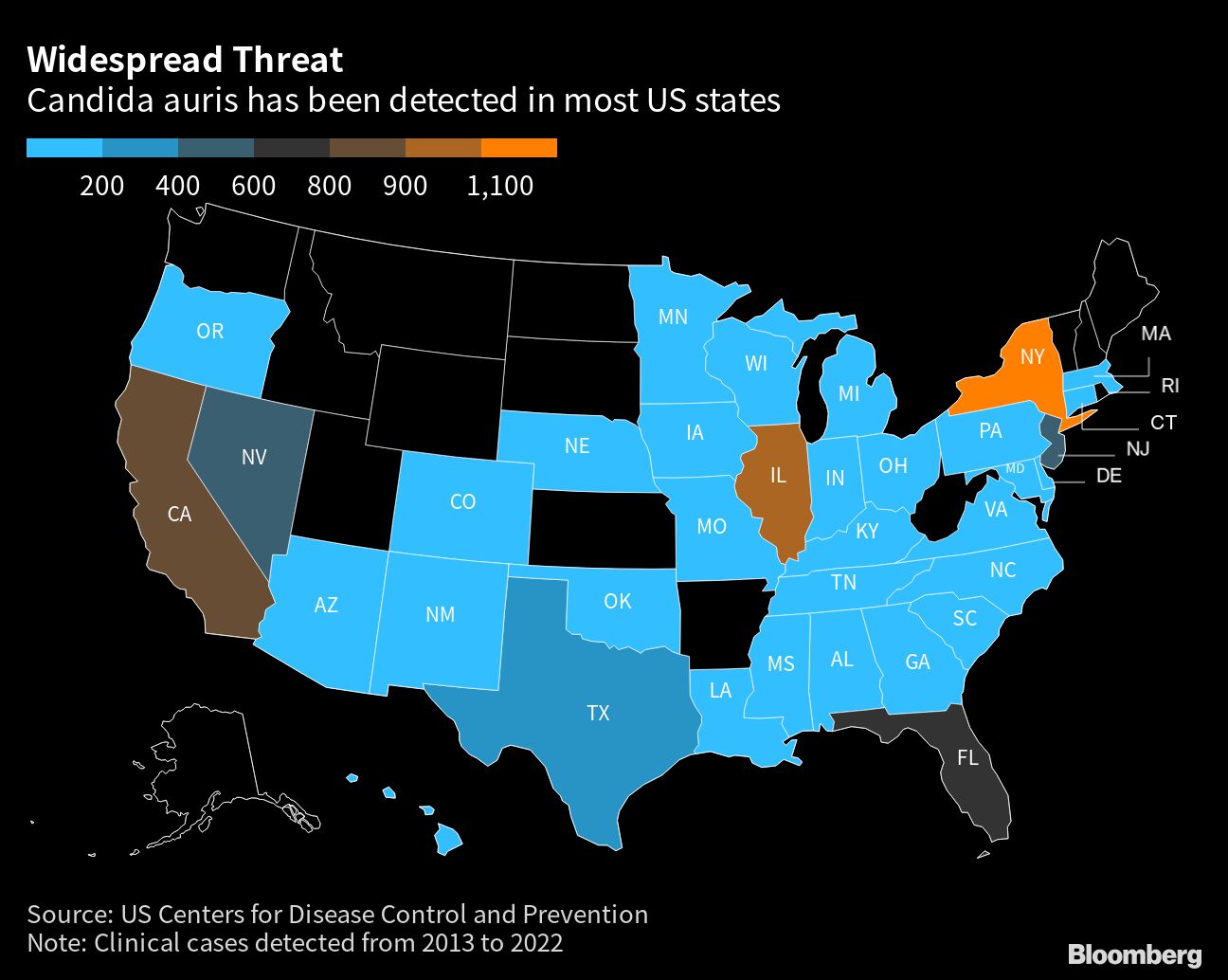
A deadly drug-resistant fungus spreading across the US saw a dramatic uptick in cases during the Covid pandemic, with more than half of all states now reporting cases.
Candida auris (C. auris) was first described in Japan in 2009, with the earliest known infections in the US dating back to 2013. Cases grew exponentially through the end of 2021, according to a paper published in the journal Annals of Internal Medicine. The Centers for Disease Control and Prevention — which says it poses a serious global health threat — noted that a further 2,377 clinical diagnoses and 5,754 cases identified through screening were reported last year.
Here’s everything you need to know about Candida auris:
How do you contract Candida auris?
Most cases of the fungus have been reported in healthcare settings, such as hospitals and nursing homes. It’s generally thought to be spread through contact with contaminated surfaces or by person to person transmission.
What does the fungus do to the body?
There are two ways Candida auris can affect the body. The fungus can either live on a specific region, such as the skin, rectum or mouth, in a process called “asymptomatic colonization,” where a patient has no symptoms but can spread it to other people. Or it can enter the bloodstream or wounds where it can cause severe invasive infections.
What are the symptoms of Candida auris?
The most common symptoms of Candida auris include fever and chills that don’t go away after treatment with antibiotics. But diagnosis is difficult as many other common diseases share those symptoms. For this reason, misdiagnosis often leads to the wrong treatment. Correct diagnosis often requires sending a blood sample or sample from an infection site to a specialized lab to definitively confirm the fungus is present.
Can it kill you?
In a word, yes, but statistics are vague. The CDC puts the mortality rate at 30-60%, based on information from a limited number of patients. But the organization cautions that many of the victims also had other serious illnesses that may have increased the risk of death.
Can Candida auris be treated with drugs?
While most infections by the fungus are treatable using antifungal drugs known as echinocandins, scientists have been worried by a rise in the number of cases resistant to the main three classes of antifungals available. That has meant physicians have had to mix multiple types of drugs at high doses to treat patients, with varying success.
Who is most at risk?
People who are already suffering from other medical conditions are often the most susceptible to the fungus, along with those who have recently stayed in healthcare settings such as nursing homes or intensive care units, according to the CDC. Invasive devices such as breathing tubes entering the body creates a potential exposure to infection. Other factors that can make someone vulnerable include recent surgery, conditions like diabetes and a broad use of antibiotics and antifungals. Healthcare officials warn that the infection has been found among all age groups.
Does the spread of Candida auris echo the plot of The Last of Us?
It’s the question everyone is asking, but the answer is no. The video game and TV series focus on a real-life fungus called cordyceps infecting humans — but in reality that fungus hasn’t made the leap to people.
Still, Arturo Casadevall, a microbiologist and immunologist at Johns Hopkins Bloomberg School of Public Health who studies how fungi cause disease, did tell Bloomberg that the fact drug-resistant Candida auris has emerged at all is “a harbinger of a scary future.”
©2023 Bloomberg L.P.







